This relapse prevention plan template should be filled out by a patient with their Behavioral Health Care Manager in the months prior to completing an episode of Collaborative Care. The purpose of a relapse prevention plan (RPP) is to remind a patient to continue doing the things that make them feel better, assess their own symptoms and warning signs, and know when to ask for more help if it is needed. In other words, a RPP is a self-management tool for patients. We also have a Relapse Prevention Plan Template available in English.
Audience: Patient
Comparing Collaborative Care to Usual Care
Introduction:
Compared with usual care, Collaborative Care has been shown to improve the effectiveness of depression treatment and lower total healthcare costs. This handout outlines those differences using data from the IMPACT trial.
A printable PDF is available for download; however, please note that this document may not conform to the WCAG-2 accessibility standards.
Comparing Collaborative Care to Usual Care
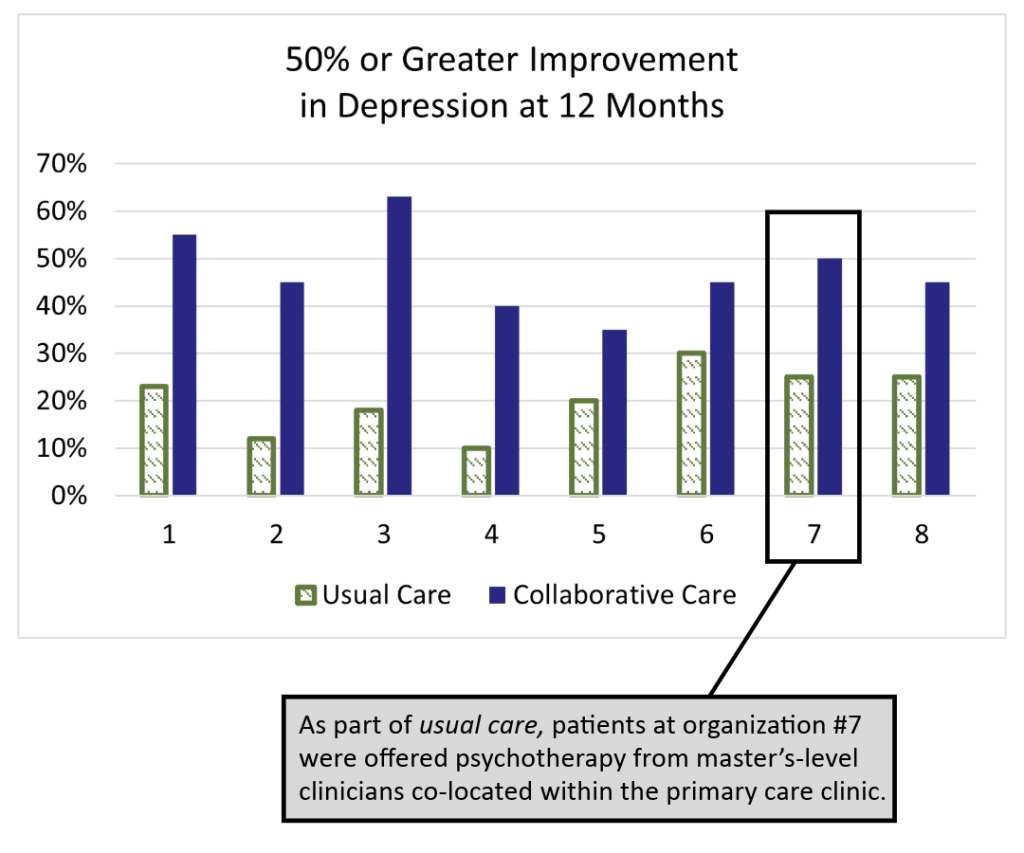
The IMPACT (Improving Mood: Providing Access to Collaborative Treatment) trial focused on depressed, older adults. Half were randomly assigned to receive the depression treatment usually offered by participating clinics, and half were randomly assigned to receive collaborative care. Collaborative care more than doubled the effectiveness of depression treatment and reduced total healthcare costs at the same time (JAMA, 2002).
Usual Care
50% of study patients used antidepressants at the time of enrollment, but were still significantly depressed.
70% of usual care patients received medication therapy from their PCP and/or a referral to specialty behavioral health.
Only 20% of patients showed significant improvements after one year, which matches national data for depression treatment in primary care.
Collaborative Care
On average, twice as many patients significantly improved. The difference was statistically significant in all eight healthcare settings. Why?
- Patient-Centered Team Care
- Population-Based Care
- Measurement-Based Treatment to Target
- Evidence-Based Care
- Accountable Care
Relapse Prevention Plan (Spanish)
Depression can occur multiple times during a person’s lifetime. The purpose of a relapse prevention plan is to help the patient understand their own personal warning signs. These warning signs are specific to each person and can help the patient identify when depression may be starting to return so they can get help sooner – before the symptoms get bad. The other purpose of a relapse prevention plan is to help remind the patient what has worked for him/her to feel better. The relapse prevention plan should be filled out by the Behavioral Health Care Manager and the patient together.
The English version of the Relapse Prevention Plan can be found here.
Relapse Prevention Plan (Generic)
The purpose of a relapse prevention plan is to help the patient understand their own personal warning signs. These warning signs are specific to each person and can help the patient identify when their mental health is declining so they can get help sooner – before the symptoms get bad.
The other purpose of a relapse prevention plan is to help remind the patient what has worked for them before to help them feel better. The relapse prevention plan should be filled out by the Behavioral Health Care Manager and the patient together.
Post Traumatic Stress Disorder (PTSD) Handout
This tool provides an overview of Post Traumatic Stress Disorder (PTSD), including symptoms, risk factors and treatment options. A Behavioral Health Care Manager can use this handout to supplement a patient’s education about PTSD.